How can we care for scoliosis and kyphosis and spondylolisthesis better with conservative care like physical therapy, high-tech scoliosis braces, exercise and other techniques? What can be done to improve surgical care, and understand choices for surgery, learning from those around the world? How can we learn from aviation and from Deming's principles of "Standard Work" to constantly improve spine and all healthcare?
Sunday, September 30, 2007
Andrea's Adolescent Kyphosis Surgery Story
Kyphosis is much less well known in the general public, and among many pediatricians and other primary care providers and OB/GYN physicians. It can be more difficult to pick up on school or physician screenings since there is no “scoliometer”-type tool to help quantify the amount of kyphotic curvature.
Improving self-image and appearance can have a HUGE effect on the life of a teenager and adult as well.
What a joy it is to see Andrea transformed, and enjoying life at a new level — an impact which will have an effect for many decades to come!
Lloyd A. Hey, MD MS
Hey Clinic for Scoliosis and Spine Surgery
Raleigh, NC USA
http://www.HeyClinic.com
ANDREA’S STORY:
Before I met Dr. Hey, I had pain in my lower back all the time. The pain got so bad that I quit playing sports, stopped going shopping, and just laid around all of the time. This was especially not good because with having Type I diabetes I needed to be exercising and I just couldn’t; I hurt so badly. I went to several doctors, trying to get an answer to my problem. Each doctor told me the same thing: I had a mild form of scoliosis and all I could do for it was conservative treatment, meaning pain pills, pain pills, and more pain pills. I even tried physical therapy and that did nothing for me. One doctor even wanted me to try anti-depressants because he said that might help. I wasn’t depressed, I just wanted help. It seemed like no one believed me about how bad my back pain really was. Then, I met Dr. Hey.
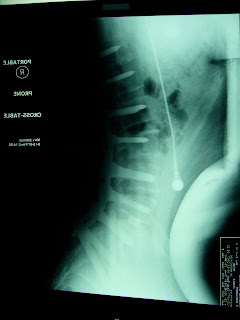
At my first appointment, Dr. Hey took x-rays of my back. When I came back to look at the x-rays he found that not only did I have scoliosis, but I had kyphosis and a degenerative disc, too, and that was the main cause of my back pain. He told me that the scoliosis, being only an 8 degree curve at the top and a 12 degree curve at the bottom, was not what was causing my problems. Dr. Hey said that my kyphosis was so severe, being an 80 degree curve, that the only solution to stopping the pain would be to have surgery. It almost seemed surreal. After going to all of the other doctors too many times to remember, I couldn’t believe Dr. Hey knew exactly what was wrong after two visits and that surgery would fix me right up.
I had surgery on December 21, 2006. Dr. Hey put two titanium rods in my back making me noticeably taller right after surgery. I was able to use my insulin pump while having my surgery to keep my glucose numbers stable. He told my mom and dad that when he first opens the back, the spine is supposed to relax, but mine didn’t because my kyphosis was so bad. Dr. Hey said a special prayer for me and eventually my spine relaxed. By the next day, I was up walking and within four days, I was back home ready to spend Christmas with my family.
The next month was difficult having to depend on someone to help me all of the time. I started to doubt having had the surgery because the pain I had healing almost didn’t seem worth it. Once I got through that first month, things started to get better. I started going back to school the full day, I started driving again, and I was feeling and looking a lot better.
It has been nine months since I had my surgery and having that surgery was the best decision I have ever made. I go shopping, go to basketball games, and have even been to the beach and been out to the ocean all without hurting and having to leave early from the pain. I went to my first prom and had the time of my life pain free. I no longer walk with my head pointed towards the ground and a hunched over back. Dr. Hey really changed my life and I can not say thank you enough to him for making me feel normal. He is a true miracle worker and I feel I have certainly had a miracle happen to me. THANK YOU DR. HEY!!!!
ANREA _________
AGE 17
Tuesday, September 25, 2007
Hey Clinic Team Photo: Happy Birthday Tracy!!
This gave us a chance to get our full Hey Clinic Team Photo!
In back row, from L to R, we have Jaclyn (PA), Jennifer (Billing), Meredith (Patient Care Coordinator), Amber (Check-Out), Melissa (Radiographic Technologist) and Tiffany (Front Desk Coordinator)
In the front row, sitting, L to R is Cathy (Practice Manager), Tracy (OR/Studies Scheduling), Brittany (PA) and me (Dr. Hey).
This team is the best group of people I have had a chance to work with in 13 years of practice, and many more years of training.
We are always working hard together to serve our existing and new patients and their families from 32 States and 4 countries who call, fax, web contact, email and visit us regularly, as well as serving the many referring physicians from around the southeast region who send us their patients as well. This is also the team which meets together weekly and for periodic staff retreats to figure out ways how we can continuously improve the quality of service to all of our “guests”, working with our hospital partners at Duke Raleigh Hospital and WakeMed Hospitals.
We want to also welcome our two most recently added team members, Amber and Tiffany who are already doing a great job. We are thankful you joined our team!
Dr. Lloyd Hey
Hey Clinic for Scoliosis and Spine Surgery
Raleigh NC USA
http://www.HeyClinic.com
29 yo woman with progressive scoliosis, who was told her curve would not progress as a teenager. How does scoliosis progress as an adult? What affect does pregnancy have on scoliosis?
Since then, she did just great until about 2-3 years ago, when she noticed that her “hourglass” figure was beginning to shift, with her R hip becoming more prominent, and her trunk sitting too far over to left, and abdomen becoming slightly more protruberant on that L side. She has had some low back pain, slightly more in past year or two.
She came in to Clinic today with questions about getting pregnant and having children with her scoliosis.
Her X-Ray shown above shows that her thoracic curve was still around 30 degrees, but her lumbar curve was now approximately 39 degrees, with severe disc collapse especially at L23 level.
She was really surprised to see the degree of progression over the past 12 years.
Why did the curve below collapse? The answer is that the asymmetric disc and facet loading over the past 12-18 years has caused an increased rate of wear of these joint surfaces. Once the discs and facet joints begin to settle and wear out, ongoing collapse can occur, which causes a vicious cycle of asymmetric loading, leading to further collapse, and so on. We use the analogy in clinic that the “car is out of alignment”, causing the “tires” (Disks) to wear out prematurely. In this young lady’s case, her spine may have been quite stable for years, then at some point the disc and facet joint wear progressed to the point that rapid curve progression and posture change occurred.
Why did her “hourglass figure” change? As the lumbar curve began to collapse, her rib cage with the upper torso “settled” down to the left side, causing the trunk to be out of alignment over the L side of the pelvis by about 3-5 cm. This causes her L side of her “hourglass” to be lost, and look possibly like a straight line, and can cause a noticable crease in the skin between the rib cage and pelvis. On the R side, since the trunk is shifting down and to the L, the R hip appears to be “sticking out”. In fact, the hip is not sticking out, but the iliac crest is more prominent since the trunk above it is shifted to the L. Her abdomen is slightly more prominent/protruberant since she has lost some height between the rib cage and pelvis, causing the abdominal contents, regardless of how many sit-ups she does, to press outward more.
Will this curve continue to progress? Only time will tell. However, her 20+ degrees of progression of this lower curve over less than 20 years combined with the degree of asymmetric disc collapse is worrisome. Careful follow-up at least is very necessary.
What about pregnancy? Pregnancy brings at least 2 major changes that could affect her comfort as well as degree of curve progression: the added weight of the baby, combined with increased ligmentous laxity throughout the body secondary to pregnancy hormone changes. These hormone changes help the pelvis to expand during delivery, but may cause laxity in the ligaments in the spine leading to increased incidence of curve progression. In terms of comfort, many women have back pain during the last trimester of pregnancy. Some women with scoliosis, especially if the curve is progressing, may have increased back and possibly leg pain / sciatica if the added weight and flexibility leads to further collapse of disc space, and neural foraminal narrowing and/or disc bulging, slippage or herniation. In my own practice, I have seen several women who have had rapid curve progression of either scoliosis or kyphosis of even 20 degrees or more during just one progression. Because of these possible issues, it is very important that all adult women with a history of scoliosis or possible scoliosis get thoroughly evaluated before getting pregnant with the first child, and also to be checked regularly between each pregnancy as well. Due to the risk of radiation on the fetus, X-Rays are not recommended during pregnancy, so any suspected scoliosis would have to be evaluated with physical examination and scoliometer only.
Could this collapse have been prevented? It is hard to say for sure, but it is possible that if the thoracic curve had been straightened and fixed when she was young, then the lumbar curve would have gone down to near zero degrees. This centering of the load may have prevented the asymmetric disc collapse in that mid-lumbar area. This possible prevention of later lumbar and/or thoracic collapse and degeneration is one of the benefits of early fixation of scoliosis in the adolescent or young adult.
Could a brace during adolescence or adulthood have prevented this collapse? No, unlikely. The brace in some growing adolescents can decrease the final curve at the time of skeletal maturity, but it does not have any protective effect thereafter for any collapse later in life that could cause ongoing progression and/or quality of life problems. Bracing typically does not improve the curve from the degree of curvature when the brace is applied — it may help to hold it closer to that number by the time they finish growing. However, if the child/adolescent is “out of alignment” at that point, as they are taken out of the brace, they still need life-long follow-up and may have later collapse of the upper or lower or both curves during adulthood — anywhere from college age, through senior citizen years.
Could earlier scoliosis have prevented this lumbar collapse? Probably yes. With modern current scoliosis techniques using pedicle screw fixation, and shorter constructs for thoracic curves (T5-L1 for example), 80-95% corrections are possible of the major curve, which results in nearly complete correction of the compensatory curves on either side, including the lumbar area. Although there can be an issue with adjacent level failure with lumbar fusions, it appears that the patients who have thoracic fusions down to L1 or L2, with most of the lumbar discs preserved actually wear their lower lumbar discs very well, especially when the top curve is well-corrected. Perhaps in the future we will have more longitudinal studies which will show that earlier short fusions can prevent the later collapse of the upper and / or lower curves that tend to affect quality of life a lot in the adult population. In this case, a “stitch in time may save nine”, in that a smaller operation can be performed on the adolescent or young adult which prevents the need for a longer instrumentation and fusion later in life to fuse across both the upper and lower curves. This younger age may also allow for a greater degree of correction, with subsequent improvement in load balance, and by fixing it at a younger age allow the discs to be subjected to more centered loads for the duration of the life of the person.
What about Self-Image and Appearance and Posture issues: are they fixable? Bracing in some adolescents can “slow” the curve progression during the growing period so the rib hump and lower hump may be smaller, but it will not make the humps go away. Bracing as an adult can sometimes help the back pain that can occur especially in the older adult with low back pain, but does not stop curve progression or self-image in most cases.
In this 29 yo patient’s situation, she is actually going to get her old X-Rays, and get a lumbar MRI so we can further evaluate the rate of progression, and also the degree of lumbar stenosis and degeneration that has already occurred.
She is considering having her scoliosis fixed prior to having her first child, since she is already concerned about the evident progression as an adult, her change in posture and self-image, and the concern about ongoing progression and degeneration which may affect her quality of life during her pregnancies and future life.
One of the interesting things about Hey Clinic is we take care people with scoliosis across the whole age range, from little children up through adolescents, young adults, middle-aged adults, and older adults. Working with this “full spectrum” of patients gives you a different perspective than just treating children alone, since the “finish line” for successful treatment for a child or adolescent is skeletal maturity with a curve less than 40 degrees for scoliosis. However, the real “finish line” for life is actually 70+ years down the line for most people, and there are many ways in which scoliosis and kyphosis can impact on quality of life during those years. As we talked about in the last Blog, there is clearly a need for further outcomes studies in scoliosis treatment, where we really try to get a handle on outcomes that really are more meaningful to patients and their families, rather than just a successful short-term radiographic measurement.
Lloyd A. Hey, MD MS
Hey Clinic for Scoliosis and Spine Surgery
http://www.HeyClinic.com
Raleigh, NC -- USA
Monday, September 24, 2007
FW: Two Years after Surgery with Hey Clinic.
From: Tim ________________
To: Dr. Lloyd Hey
Sent: Mon Sep 24 14:10:54 2007
Subject: Two Years
Hello Dr. Hey, on September 19th I reached a major
milestone, that being my two year anniversary of
having you fix my chronic back problem. Truthfully, I
can not think of any restriction I place on myself
beyond just good common sense. I have learned to take
my time and lift or do things in a smart manner or
heavens to bid, ask for assistance! The quality of my
life has changed so dramatically this past year it is
truly amazing. I remember those moments along the
healing path when I thought, "will I every get beyond
this point" but time and exercise will get one there.
While I was never a good golfer, Nancy and I play
several evenings a week and we always walk with our
push carts and I'm playing the best golf of my life.
I even won the long ball contest during a local fund
raiser by tying our Pro with a 326 yard drive.
My Daughter Erica is making incredible progress on her
post surgery healing (Dec 06) and I keep reminding her
to just give it time. She and I are blessed to have
met you and to have had you work your wonders on our
troubled backs. We will always be appreciative and
thankful for all you and your fantastic staff have
done for us.
Thank you and God bless.
Sincerely,
Tim _________________
------ End of Forwarded Message
Dr. Hey's speciality: Orthopaedic or Neurosurgery Spine?
My residency training and pediatric scoliosis and pediatric orthopaedic training was at Harvard Combined Orthopaedic Surgery Program and Boston Children’s Hospital.
My adult fellowship training at Duke was in both Neurosurgery and Orthopaedic Spine.
My Board Certification, including recertification this year is with the American Board of Orthopaedic Surgery.
When I served on faculty at Duke for approximately 10 years, I taught in both neurosurgery orthopedic surgery residents and fellows.
On a day to day basis, I do complex spinal nerve, spinal cord, and deformity corrective surgery, as well as complex revision surgery 4 days a week, and have done nearly 5,000 surgeries over past 13 years of practice, on both children and adults, here in Raleigh and Duke Medical Center.
I look forward to meet you!
Dr. Hey
On 9/24/07 11:10 AM, "Rebecca wrote:
I have an appointment with Dr. Hey this Thursday and had a question. Could you tell me please, is Dr. Hey a neurosurgeon or an orthopaedic surgeon??
Thank you,
Rebecca _________________
------ End of Forwarded Message
Sunday, September 23, 2007
Natural History of Adolescent Scoliosis Curve Progression as a Function of Degree of Curvature and Age. Scoliosis Bracing Decision Requires More Information and Dialogue, not simple rule.
If there is any significant growth remaining, consider putting the child/adolescent in a brace if:
- Cobb angle 30-39 degrees on initial presentation, or
- Cobb angle 25-30 degrees with documented progression, (meaning that you had a previous X-Ray showing Cobb Angle less than 25)
As a resident we loved simple rules, since it made life so much simpler for everyone. Once we knew how to measure the Cobb Angles accurately on the X-Ray using our grease pencils and goniometers, we could successfully determine the treatment:
- Observe (Cobb < 25)
- Brace (Cobb 25-39)
- Surgery (Cobb 40-45 or more)
What could be simpler? Measure Curve. Order Brace. “Next!”
However, after spending two and a half years at Children’s from 1989 through the spring of 1994 off and on as Junior Resident, Senior Resident, Fellow, and then Chief Resident I began to realize that things were not quite so cut and dry as I initially thought. Now, some 13+ years later after finishing up as Chief Resident at Children’s, and having cared for thousands of patients with spinal deformities since then, and also combined with having 2 kids of my own who are now both teenagers, it has become clear that using the simple rule “stamp” to fly through clinic just doesn’t cut it. In addition, after getting additional training in epidemiology at the Harvard School of Public Health, I began to be able to see some of the deeper strengths and weaknesses in the existing scoliosis bracing and other treatment outcomes studies.
Last week at Hey Clinic I saw a very pleasant 9 yo girl with a 28 degree thoracic scoliosis as a second opinion regarding bracing vs. observation vs. other treatment.
We had a good long talk about many of the issues regarding the natural history of scoliosis progression during childhood and adolescence, and also about the long-term effects of scoliosis, including the risk of progression in adulthood.
One of the statistics that I shared with them was that the chance of significant curve progression was very dependent on the size of the curve combined with the number of years remaining for growth. In this child’s case, at age 9 or 10, she has at least 6 more years of growth remaining. Back in 1982, the Scoliosis Research Society (SRS) presented a natural history paper at the Denver SRS Annual meeting which included the Table shown above. In this table, you can see how the younger you are and the bigger your curve, the more likely you will have curve progression. In this girl’s case, she would have over a 90 percent chance of curve progression based on this data. This would be in great contrast to the 16 yo girl who would have a much lower chance of progression.
Attached is a photograph of a data table from Stuart Weinstein’s textbook “The Pediatric Spine” , Chapter 21, “Natural History of Adolescent Idiopathic Scoliosis, page 466, which is:
Table 2. Probability of progression: Magnitude of curve at initial detection
versus age
Curve
Magnitude
at Detection Age at Detection
10-12 y 13-15 y 16 y
< 19 deg. 25% 10% 0%
20-29 60 40 10
30-59 90 70 30
>60 100 90 70
from Weinstein's "The Pediatric Spine", p 466, Table 2, quoted from reference
78, Nachemson, a, Lonstein J, Weinstein S (1982): Report of the SRS
Prevalance and Natural History Committee 1982, reported at 1982 SRS Denver.
In this chapter, Stu Weinstein outlines 4 growth factors, and 2 curve factors that have big impact on predicting curve progression:
- Younger the patient at age of diagnosis
- Greater risk of progression before the onset of menarche in females.
- The lower the Risser grade at curve detection, the greater the risk of progression. (Your daughter is at lowest Risser grade 0 — ossification of iliac crest growth plate)
- Males are at 1/10 of risk progression than females.
2 curve factors:
- Double curve patterns have greater tendency to progress than single
- Larger magnitude of curve at detection, the greater the risk of progression (11 references quoted)
In this chapter they also report from Univ Iowa study that thoracic curves more than 30 degrees at maturity progressed an average of 19 degrees during the 40 yr f/u period, with the fastest progression being in the curves that were 50-75 degrees at time of maturity, which progressed 0.75 to 1 degree per year (40 degrees over 40 yrs).
This huge variation in expected progression is one of the reasons why it is difficult to interpret many of the bracing studies, in terms of their effectiveness of treatment, since many of these studies included a large percentage of adolescents who were in this low risk of progression group.
However, there have been several recent studies which have called into question the clinical effectiveness of scoliosis bracing, and have strongly suggested the need for new randomized control trials (RCT) to better understand when the Boston Brace or other braces can be useful for preventing curve progression (see below). I can tell you with my own background in epidemiology and outcomes research, it is very difficult to study the effectiveness of bracing for several reasons:
- There is tremendous variation among children and adolescents who present with scoliosis in terms of:
-- age at presentation
-- curve size at presentation
-- growth rate
-- curve flexibility
2. Variations in treatment
-- type of brace, if any
-- hours brace worn
-- tightness/fit of brace
-- number of months of treatment
3. Difficulties in getting long-term follow-up data.
-- relatively rare disease.
-- takes MANY YEARS (maybe even 40 or more) to get the outcome you truly care about, which is long-term quality of life THROUGH adulthood, versus the typical short-term measure typically used which is 5 degrees of progression. The current outcome measure of “successful bracing” of 5 degrees or less of progression during a relatively short time period of 2 years after reaching skeletal maturity has more to do with the practical issue of having a measurable outcome variable within the lifespan of many of the investigators that are doing the study, and also while the patients can still be tracked for follow-up. Understanding what the investigators are considering “successful outcome” versus what we would like to know as a life-long “successful outcome” is an important distinction.
-- Many patients “cross over” to surgical treatment once their curve shows progression.
In addition, it is important for the child and family to realize the following:
- In order for the brace to be effective, it must usually be worn from 16-23 hours per day.
- Compliance can often be an issue, and can create tension between child and parents.
- The brace must be worn until skeletal growth is completed, which could be 2-6 or so years in most cases.
- There may be some psychological / self-image issues around brace wear that could effect the child’s development.
- There is no guarantee that the brace will work. Scoliosis surgery may still be necessary as an older adolescent, young adult or older adult. Some adolescents feel “cheated” if they choose the bracing option, and then end up needing surgery anyway. I have had college students weeping wildly in my office, who were treated for years in a brace through middle school and high school who then found out that they needed scoliosis surgery anyway.
- The braces can be very expensive (often over $2,000 - $5,000) from most orthotists, although usually covered at least in part by insurance.
- Bracing usually multiple trips to orthotist for adjustments, and possibly new braces required as the child grows.
- Additional X-Rays needed in the brace to judge the effectiveness of the brace on curve correction.
- Bracing does not improve the appearance of the deformity, or the end curve measurement — the hope is to hold the curve at or near the current measurement. Self-image issues have been shown to be a major factor in the long-term effect of scoliosis on the individual.
- Scoliosis surgery has changed a lot during the past 40 years, with excellent improvements in postural appearance, much shorter surgical times, hospitalizations, and recovery times, and lower complication rates.
- Bracing may be helpful to at least delay surgery until a child is bigger, and has had more axial growth, making surgery less risky. However, this has to be weighed against the potential for severe curve progression despite brace.
- Other factors may affect the child/adolescent’s ability to be successfully braced, including body habitus and curve flexibility and location.
Therefore, rather than just applying a simple formula to the decision for bracing a child with scoliosis, we feel that it is better to have a longer dialogue discussing many of the issues above, and then personalizing the treatment based on the particular child/adolescent and their family. This often takes quite a bit of time for me and/or my physician assistants to have an un-rushed encounter or series of encounters to weigh the pros and cons and make the best possible decision for their child/adolescent and family. Like many things in life, there is often no “Black or White” clear answer, but many factors that need to be considered — which should not be too surprising given the complexity of the human body, human spine, and the growing adolescent child in a family and social environment. Hopefully in the future, as we understand the genetic and other etiologies of scoliosis better, and have improved prospective studies we should be able to counsel our patients and families even better. The learning never ends.
Dr. Lloyd Hey
http://www.HeyClinic.Com
Hey Clinic for Scoliosis and Spine Surgery
Raleigh, NC -- USA
Some recent abstracts regarding scoliosis bracing are found below, and can also be found by searching http://www.pubmed.org
========
A comparison of the thoracolumbosacral orthoses and providence orthosis in the treatment of adolescent idiopathic scoliosis: results using the new SRS inclusion and assessment criteria for bracing studies.
Janicki JA, Poe-Kochert C, Armstrong DG, Thompson GH.
Division of Pediatric Orthopaedics, Rainbow Babies and Children's Hospital, University Hospitals of Cleveland, Case Western Reserve University, Cleveland, OH 44106, USA.
This is a retrospective cohort study comparing the effectiveness of the thoracolumbosacral orthosis (TLSO) and the Providence orthosis in the treatment of adolescent idiopathic scoliosis (AIS) using the new Scoliosis Research Society (SRS) Committee on Bracing and Nonoperative Management inclusion and assessment criteria for bracing studies. These new criteria will make future studies comparable and more valid and accurate. METHODS: We have used a custom TLSO (duration, 22 hours/day) and the Providence orthosis (duration, 8-10 hours/night) to control progressive AIS curves. Only 83 of 160 patients met the new SRS inclusion criteria: age of 10 years and older at initiation of bracing; initial curve of 25 to 40 degrees; Risser sign 0 to 2; female; premenarcheal or less than 1 year past menarche; and no previous treatment. There were 48 patients in the TLSO group and 35 in the Providence group. The new SRS assessment criteria of effectiveness included the percentage of patients who had 5 degrees or less and 6 degrees or more of curve progression at maturity, the percentage of patients whose curve progressed beyond 45 degrees, the percentage of patients who had surgery recommended or undertaken, and a minimum of 2 years of follow-up beyond maturity in those patients who were thought to have been successfully treated. All patients are evaluated regardless of compliance (intent to treat). RESULTS: There were no significant differences in age at brace initiation, initial primary curve magnitude, sex, or initial Risser sign between the 2 groups. In the TLSO group, only 7 patients (15%) did not progress (<or=5 degrees), whereas 41 patients (85%) progressed by 6 degrees or more, including the 30 patients whose curves exceeded 45 degrees. Thirty-eight patients (79%) required surgery. In the Providence group, 11 patients (31%) did not progress, whereas 24 patients (69%) progressed by 6 degrees or more, including 15 patients whose curves exceeded 45 degrees. Twenty-one patients (60%) required surgery. However, when the initial curve at initiation of bracing was 25 to 35 degrees, the results improved. Five (15%) of 34 patients in the TLSO group and 10 (42%) of 24 patients in the Providence group did not progress, whereas 29 patients (85%) and 14 patients (58%), respectively, progressed by 6 degrees or more, and 26 patients (76%) and 11 patients (46%), respectively, required surgery. CONCLUSIONS: Using the new SRS bracing criteria, the Providence orthosis was more effective for avoiding surgery and preventing curve progression when the primary initial curves at bracing was 35 degrees or less. However, the overall success of orthotic management for AIS in both groups was inferior to previous studies. Our results raise the question of the effectiveness of orthotic management in AIS and support the need for a multicenter, randomized study using these new criteria.
PMID: 17513954 [PubMed - indexed for MEDLINE]
Related Links
* Nighttime bracing with the Providence brace in adolescent girls with idiopathic scoliosis. [Spine. 2001]
* Standardization of criteria for adolescent idiopathic scoliosis brace studies: SRS Committee on Bracing and Nonoperative Management. [Spine. 2005]
* Effectiveness of the SpineCor brace based on the new standardized criteria proposed by the scoliosis research society for adolescent idiopathic scoliosis. [J Pediatr Orthop. 2007]
* A comparative study of TLSO, Charleston, and Milwaukee braces for idiopathic scoliosis. [Spine. 1998]
* Results of brace treatment of scoliosis in Marfan syndrome. [Spine. 2000]
See all Related Articles...
Display Show
-------
Professional opinion concerning the effectiveness of bracing relative to observation in adolescent idiopathic scoliosis.
Dolan LA, Donnelly MJ, Spratt KF, Weinstein SL.
Department of Orthopaedics and Rehabilitation, University of Iowa Health Care, Iowa City, IA 52242, USA. lori-dolan@uiowa.edu
OBJECTIVE: To determine if community equipoise exists concerning the effectiveness of bracing in adolescent idiopathic scoliosis. BACKGROUND DATA: Bracing is the standard of care for adolescent idiopathic scoliosis despite the lack of strong reasearch evidence concerning its effectiveness. Thus, some researchers support the idea of a randomized trial, whereas others think that randomization in the face of a standard of care would be unethical. METHODS: A random of Scoliosis Research Society and Pediatric Orthopaedic Society of North America members were asked to consider 12 clinical profiles and to give their opinion concerning the radiographic outcomes after observation and bracing. RESULTS: An expert panel was created from the respondents. They expressed a wide array of opinions concerning the percentage of patients within each scenario who would benefit from bracing. Agreement was noted concerning the risk due to bracing for post-menarchal patients only. CONCLUSIONS:: This study found a high degree of variability in opinion among clinicians concerning the effectiveness of bracing, suggesting that a randomized trial of bracing would be ethical.
PMID: 17414008 [PubMed - indexed for MEDLINE]
Related Links
* The objective determination of compliance in treatment of adolescent idiopathic scoliosis with spinal orthoses. [Spine. 2006]
* Standardization of criteria for adolescent idiopathic scoliosis brace studies: SRS Committee on Bracing and Nonoperative Management. [Spine. 2005]
* A meta-analysis of the efficacy of non-operative treatments for idiopathic scoliosis. [J Bone Joint Surg Am. 1997]
* Effectiveness of braces in mild idiopathic scoliosis. [Spine. 1984]
* A comparative study of TLSO, Charleston, and Milwaukee braces for idiopathic scoliosis. [Spine. 1998]
See all Related Articles...
Display
-- Phys Ther. 2005 Dec;85(12):1329-39.Click here to read Links
Comment in:
Phys Ther. 2007 Jan;87(1):112; author reply 112-3.
Effect of bracing and other conservative interventions in the treatment of idiopathic scoliosis in adolescents: a systematic review of clinical trials.
Lenssinck ML, Frijlink AC, Berger MY, Bierman-Zeinstra SM, Verkerk K, Verhagen AP.
Department of General Practice, Erasmus Medical Centre Rotterdam, PO Box 1738, 3000 DR Rotterdam, The Netherlands.
BACKGROUND AND PURPOSE: Many conservative treatments are available for adolescents with idiopathic scoliosis, but the evidence for their accepted use is still unclear. The purpose of this study was to evaluate the effectiveness of braces and other conservative treatments of idiopathic scoliosis in adolescents by systematically reviewing the literature. METHODS: The literature was searched in the PubMed, CINAHL, Cochrane, and PEDro databases. Studies were selected if the design was a randomized clinical trial or a controlled clinical trial, if all patients had an idiopathic scoliosis, if all patients were less than 18 years of age during the intervention, and if the type of intervention was a conservative one. Two reviewers independently assessed the methodological quality using the Delphi list and performed data extraction. Analysis was based on the levels of evidence. RESULTS: Thirteen studies met the final inclusion criteria, showing a wide range of interventions such as bracing, electrical surface stimulation, and exercises. DISCUSSION AND CONCLUSION: The authors conclude that the effectiveness of bracing and exercises is not yet established, but might be promising. They found no evidence of the effectiveness of electrical stimulation.
PMID: 16305271 [PubMed - indexed for MEDLINE]--------
Duke Pre-Med Student, Jing, shares some reflections on her summer "shadow" internship experience with Hey Clinic
My Experience at the Hey Clinic
When Duke University’s Health Careers Exploration Program first informed me that I would be shadowing Dr. Hey in the Hey clinic this past summer, I was so excited. I started looking through the clinic’s website, and reading the blogs online. I hadn’t ever heard of a spinal clinic before and was really interested to learn more.
On the first day that I was supposed to be shadowing, I was very nervous, but everyone was so friendly and welcoming that I immediately started feeling more comfortable. It was an eye opening experience for me to be in the clinic and to meet some of the patients with scoliosis, kyphosis, spinal stenosis, spondylolisthesis, disc herniations and other spinal problems because I’ve always had the idea that only the elderly experienced spinal issues. I had no idea that the same problem could occur in otherwise healthy children and adults.
When I first started listening to the patients in clinic about what their symptoms were, it just amazed me that some of them had been living with their symptoms for years. For example, there was one woman in her 60s who had not been able to stand for more then 10 minutes and could not walk for more then 50 yards, and had lived like that for over 5 years. I could not imagine myself not being able to sit down for more then 10 minutes at a time, which I am sure caused even more pain for her besides her normal back pain.
I think the patient that stands out the most in my mind was little 12-year-old Heather who had a very sever double curve scoliosis. She just seemed so healthy and full of life that I could not see her having such a serious spinal deformity, and the speed with which it developed (they only noticed a slight scoliosis a year before) also shocked me. The shock, fear and confusion that you could see in her parents’ touched me deeply because I could imagine how my parents would have felt if they had just found out a week ago that their daughter had scoliosis and suddenly a week later she was being scheduled for surgery and would have a metal rod in her back for the rest of her life. Any yet I was just as equally impressed with the calmness that the parents presented in front of their daughter in order to make Heather feel better and how brave Heather was about the whole thing. I also think that because I was there for the families’ entire Hey clinic experience (I was there for her first check-up at the clinic, during her surgery and for post-op, and I even saw her before and after x-rays) it made me feel closer to them and more able to empathize with their situation.
If you had asked me two years ago, what field of medicine would I want to go into, I would have told you: “not surgery.” But my thoughts on that have started to change in the past two years; so for me, the opportunity to observe the surgical side of the Hey Clinic was an invaluable experience. Sitting in the surgical room with the high definition camera pointed at the surgical area gave me a perfect view of everything without making me nervous about possibly being in the way. It was also amazing for me to see Dr. Hey working on the patients, especially when I had a spine model in front of me because I could see on the model how small of an area was available for the pedicle screws and yet he was able to get them all in fast and efficiently. It was especially incredible because from my point of view much of the anatomy looked the same and I sometimes couldn’t tell the tissue and muscle from the bone. What also surprised me was the amount of force used in surgery, I had never envisioned surgery on something as delicate (by delicate I don’t mean something that is fragile and easily broken like glass, but rather something that if broken would have serious consequences) as a spine would involve so much pushing, bending, cutting, and drilling. The whole Hey Clinic experience only reaffirmed my desire to go into medicine and has made me consider surgery as a definite field of interest.
Jing
Thursday, September 20, 2007
Anterior/Posterior (A/P) spine reconstruction for 50 yo woman with flatback syndrome, and L5S1 severe disc collapse below previous long fusion, with removal of unusual hardware. Hey Clinic Surgery Sep 20 2007. Spine Surgeon Surgical Tips: Instruction Manual for Removing Grubb Spinal Hardware.
We ended up fixing this woman’s degenerative disc and “flat back” problem by doing an anterior/posterior or “A/P” or “front and back” spinal procedure. First, working with Dr. Chris Watters from General Surgery here in Raleigh we went in through her abdomen through a small transverse “bikini” incision, and exposed the L5S1 disc from the front. I scraped out the disc, which was really completely gone, with bone rubbing on the bone. I distracted open the space, roughed up the bony surfaces, and removed the small amount of residual disc toward the back. I then inserted a titanium anterior lumbar interbody fusion (ALIF) cage, which is the blue cage pictured above, packed with bone. These cages come in a variety of sizes. By putting a special “jack” to lift open her L5S1 space, I was able to open the anterior L5S1 disc space from zero mm up to 15 mm anteriorly, and then slip in the 15 mm ALIF cage with bone graft. The ALIF cage is shaped like a wedge, to help recreate the proper lordosis, or backward curvature that the lumbar spine is supposed to have. Very small improvements in this angle at L5S1 can have HUGE effects on the center of gravity of the patient, just as jacking up one side of the leaning Tower of Pisa has a huge effect on the displacement of the floors a hundred feet or more above. I then put a screw with a washer into the S1 vertebra to prevent the cage from migrating after surgery. The anterior wound is then closed up with a plastic surgery-type subcuticular closure, and then the patient is turned to the prone position to fix the posterior part of the spine.
The next big challenge is to remove the old hardware. Today we have a special challenge.
How to Take Out Grubb Spinal Hardware.
Her hardware is not a commonly used pedicle screw system invented by a Dr. Grubb who used to work at Durham Regional years ago. This system is very difficult to remove, so if this X-Ray looks familiar, and you are a spine surgeon planning a revision, you may want to see one of my old Blogs in my archive from last year for some tips on hardware removal, or check out my “Tips” below. As my senior residents said at the Brigham and Mass General Hospitals: “You Never Look Good Taking Out Hardware”! This is definitely true when you are trying to remove Dr. Grubb’s custom hardware. The defining characteristics of the Grubb hardware is the unusual “rough rod”, combined with an unusual pedicle screw to rod connector that appears as a big rectangle on X-Ray. Do not bother trying to contact the vendor or Durham Regional Hospital to get the tools for extraction — there are none.
Here is a list of the tools you will need to get this system out:
- Large Bolt Cutter. You need to cut the rod between every pedicle screw, very often.
- 1/2 inch curved osteotome to get the bone away from around the pedicle screws and other hardware, and also to pry off the initial top small wire on the top of each pedicle screw connector.
- Large fragment Synthes screw driver to take out the pedicle screw,
- Small head universal driver to remove the approximately 5mm nut on the top of the pedicle screw connector.
- A lot of patience.
- High speed burr can be helpful as well.
Here are some tips on how to get it out.
Expose the hardware and overlying bone.
Chisel out the bone from around the rod and pedicle screw connectors. The pedicle screws may be quite a ways away from the connecting rod.
Chisel off the top small piece of wire which holds on a rectangular piece of metal that prevents the top nut from loosening.
Chisel off the top rectangular piece of metal with the chisel.
Loosen nut on top of pedicle screw connector. The connector should gradually lift off. Sometimes you can cut the connector below the rectangular metal piece.
Cut the rods between each pedicle screw so you can slip out the pieces of rod. This could be many cuts.
Now you are going to look in there and just see some little threaded pieces of metal sticking out of the fusion mass and wonder where the pedicle screws are.
The answer is this: The pedicle screws are connected to that little piece of threaded rod, but not directly below it. Instead, the pedicle screws have a large, flat head, about 1/2 inch in diameter with the Synthes female hex hole in the middle of the screw. On the edge of that 1/2 inch circle is attached the vertical threaded post that you see sitting out of the bone. So now what you have to do is to chisel down and around that vertical post at every level, and find that 1/2 inch flat circular top of the pedicle screw. You may literally have to explore 360 degrees around each post to find the top of the pedicle screw, which can take a while. Now it gets even worse. At this point when you have that 1/2 inch shiny metal top of pedicle screw, and you get your Synthes screw driver in the middle of it, but when you go to turn it, it won’t turn. At this point, you may say something bad. Hold your tongue. Here’s the problem. While the huge pedicle screw top looks round, it actually is not completely round, since the vertical post actually sticks out slightly from the circumference of the big pedicle screw head. Therefore, when you go to turn it in bone, this acts like a lock, and prevents screw turning. To solve this, you need to chisel some more (or use burr) , down and around the head of the screw, giving yourself a 2-4 mm extra diameter opening another 3-4 mm deep. Now when you go to turn the Synthes screwdriver, the pedicle screw unscrews. At this point the Halleluiah Chorus begins to sing all around you, as you lift the last piece of evil hardware from the patient, feeling a bit like Indiana Jones outsmarting the Temple of Doom. All kidding aside, my Surgical assisting PA Brittany helped me keep my sanity on our last Grubb hardware removal case by giving an enthusiastic “Woo Hoo!!!” after every screw I successfully removed. There were about 12 screws to come out, so there was a lot of “Woo Hooing” going on!
After we removed her old hardware, we put in new hardware from L2-Iliac wing bilaterally. This was a bit challenging since both of her iliac crests have been used for her previous 6 spinal fusions, with most of the posterior iliac crest on the R side removed. On the L side I was able to get a great passage down the remaining iliac crest, but on the L side had to use some of the sacrum combined with SI joint for the most distal set of screws. Long iliac wing fixation when combined with Sacral screws provides a very strong foundation for these high stress long constructs.
I then did a posterior osteotomy of L5, removing the entire lamina and pars so that I could “close the book”, and create additional lumbar lordosis by closing down the posterior part of the spine. Putting the OR table into a “V” position, as well as taking time to contour your rods to maximize the lumbar lordosis is very helpful. I was able to create an additional 15-20 degrees of lordosis this way. We did not have to hook our instrumentation to the old instrumentation above since there was a very solid fusion in between these two areas of hardware. The old fusion mass as well as the sacrral ala are roughed up to help bone healing and bone graft is packed out over this decorticated bone to promote the necessary new fusion. A special three cross-connector system is used to help decrease bending loads around the sacral screws.
Total surgical time was six hours 45 minutes. EBL 2200 cc. 2 units of PRBC transfused in addition to cell saver. Patient is doing well tonight recovering in ICU extubated. Husband very happy.
So what can we learn from today?
- One way to fix flat back syndrome is by “jacking up” the disc or discs that have collapsed with ALIF cages, combined with posterior osteotomies and hardware.
- You never look good taking out hardware.
- Always be prepared to have right equipment to take out hardware, which always includes a large bolt cutter, chisel and burr.
- If you are a young spine surgeon trying to figure out what instrumentation to use, please consider the “ease of removal” issue, as well as the “ease of adding on” or extending a fusion with connectors, etc. It might make your life, or the life of your patient and another surgeon much more pleasant and less risky in the future.
- You can get in pelvic hardware like iliac wing screws in patients who have had iliac crest bone graft removed, but study your CT scan of pelvis preop, and be willing to adapt a little if there is not enough bone on both sides.
Tomorrow we will get this young lady standing up for first time, with her center of gravity back where it belongs, and without the raw bone rubbing on raw bone at L5S1. I have had many patients with this problem tell me that they feel like the “top half of their body is not well connected to the bottom” when walking, or changing position. Some can even feel a “clunk”, often painful when changing position as the L5 slips on S1. Well, now her top half is well connected to the bottom, and the nerves in between are no longer being crushed. There is hope for renewed quality of life despite her long history of many spine surgeries.
Lloyd A. Hey, MD MS
http://www.HeyClinic.com. em: hey at heyclinic.com
Hey Clinic for Scoliosis and Spine Surgery
Raleigh, NC USA
Wednesday, September 19, 2007
Oklahoma 40 yo gentleman Kyphosis causing neck and low back pain

On Friday I saw one of my patients from Oklahoma back for follow-up. He is about 40 years old, and has suffered with an accentuated thoracic kyphosis for many years. The curve has not progressed over past 4-6 years, with a thoracic curve around 59 degrees, which is certainly above normal, but has not progressed recently. He works in the financial sector, and travels a lot. He has noticed increasing problems with lower back and neck pain over the years.
Why would the neck and low back hurt, if the deformity is in the thoracic spine?
Well, the answer is that some patients with increased thoracic kyphosis have no pain, and some have pain over the thoracic deformity, while others have pain in the neck or low back area or both. The reason for the neck and/or low back pain is that these areas have to “compansate” for the thoracic increased kyphosis by curving backward more into what we call “Lordosis” (the opposite of kyphosis). This accentuated lordosis can cause increased pressure on the posterior elements including the facet joints. As people get a little older, these facet joints get a bit arthritic, and can be painful if the neck or low back are forced to stay in a “hyperextended” position due to the necessary compensation for the structural thoracic curve.
We are going to try a round of conservative treatment for our friend from Oklahoma.
However, if his curve progresses, or his pain continues to increasingly affect his quality of life, then we may have to consider fixing his thoracic kyphosis.
In the past blogs and podcasts, I have shared some interviews with one of my patients from Chicago IL who had a 90 degree thoracic kyphsos with severe neck pain, who had complete relief of her neck pain and a totally changed posture and self-image after her thoracic kyphosis was corrected. Her podcast interview can be found through iTunes by searching for Dr. Hey’s Podcasts, or through my old Blod and Video Podcast site at http://web.mac.com/drhey. For some reason this hot link to this archived web.mac account does not work, but if you copy or type in URL, you will have no trouble.
17 yo girl who had her kyphosis fixed can be found recently on this blog.
Lloyd A Hey, MD MS
http://www.heyclinic.com
Hey Clinic for Scoliosis and Spine Surgery
Raleigh, NC USA
Big Kyphoscoliosis and Herniated Disc Repair in 30 yo woman from Virginia. Hey Clinic Surgery Sep 19 2007
She had 2 previous laminectomies done down at L45 and L5S1, and actually had her symptoms get much worse after these surgeries, and also had worsening of the scoliosis. Laminectomies can destabilize the spine, and accelerate collapse of scoliosis when not combined with surgical fusion stabilization. Her pain was so bad down her R leg that she literally limped around the hospital.
Maggie’s surgery went very smoothly today. She had a combination of thoracolumbar scoliosis and a thoracic and thoracolumbar junction kyphosis. Because of her large symptomatic recurrent disc herniation at L5S1, I needed to fix this bottom disc level as a part of the overall reconstruction. We fixed her spine from T3 above in the thoracic spine, down to S1 and the Iliac Wings down at the lower spine and pelvis. I had to do a complex revision decompression of the nerve roots of L4, L5 and S1 which were all socked in with scar, and being compressed by herniated disc and enlarged facet joints. I replaced the herniated disc at L5S1 shown in the MRI axial view above with a TLIF transforaminal interbody cage and bone graft. This provides interbody support at the bottom of the construct, which is very helpful to promote fusion and stability when combined with the posterior instrumentation down to the iliac wings.
Her bone quality was excellent because of her young age, which made the pedicle screws more difficult to place, but will make the screws much less likely to loosen. That is one reason why it is better to get scoliosis or kyphosis corrected when the patient is younger, rather than older, since the quality of the bone (level of osteoporosis) is much better in younger people, and the bone heals more rapidly in younger people.
Maggie’s surgery took about 6 hours today, and required no transfusions intra-operatively. Her intraoperative radiographs show nice correction of her scoliosis and kyphosis. I did attach the bottom iliac wing screw on R after the X-Ray was taken, and added a couple cross-links for additional stabilityI did give her 2 units of PRBC’s postoperatively in PACU. She is doing very well postoperatively in ICU overnight. Her husband was extremely thankful.
Tomorrow she’ll get up and around. We had a wonderful “Gem” new nursing graduate named Brittany in observing surgery today on our “big screen” monitor hooked up to our special operating room sterile overhead light. Brittany learned a ton about scoliosis surgery today and spinal anatomy today, and did very well on the “pop quiz”! We hope Brittany will join our awesome inpatient orthopaedic spine scoliosis service at Duke Raleigh Hospital!
Lloyd A. Hey, MD MS
Hey Clinic for Scoliosis and Spine Surgery
Raleigh, NC — USA
http://www.HeyClinic.com
Monday, September 17, 2007
What does a Decompressed Dural Sac (Spinal Canal) Look Like After Laminectomies? Surgery Video Sep 17 2007 Dr. Lloyd Hey, Hey Clinic
In this short 30 second video, I show the dural sac exposed from T12 down to L5. A neurosurgical "sucker" is on the R side of the screen. Pedicle screws can be seen on either side. A bent metal probe called a "Ganz 4" is then gently passed out each of the nerve holes on each side, called the neural foramen to ensure that our decompressive laminectomy is complete, including the central area, lateral recess, and neural foramen.
This is the point in the case where if you listen real hard you can hear the nerves go "Ahhhh..."
Tomorrow this gentleman will be standing up and starting walking with better posture and hopefully less leg pain as the nerves recover.
Spinal Stenosis Above Previous Fusion. Sept 17 2007 PM Surgery
His CT scan shows stenosis at the 2 levels above hhis existing fusion, and possibly some residual stenosis L2-5.
Today, I removed the old hardware, explored the fusion, and extended the fusion up to T12.
I then decompressed the dural nerve sack from T12 all the way down to L5, including removing residual bone spurs, ligament and scar.
His X-Rays are shown here, and the next blog shows a short video of the dural sack fully decompressed, and palpating out the neural foramen at each level using a special tool called a “Ganz 4”.
His nerves are now fully decompressed, and spine stabilized.
He did very well during the surgery, which took approximately three hours and 45 minutes.
Estimated Blood Loss (EBL) was 450 cc, and he did not require a transfusion.
He was doing well in the PACU for my postoperative check this evening, and will get up and around tomorrow.
Lloyd A. Hey, MD MS
Hey Clinic for Scoliosis and Spine Surgery
http://www.HeyClinic.com
Spondylolysis and Spondylolisthesis L5S1: Corrective Surgery Sep 17 2007 AM. Dr. Lloyd Hey, Hey Clinic
His X-Ray shows a slight lucency posteriorly at L5 where the stress crack is located, but it is hard to see.
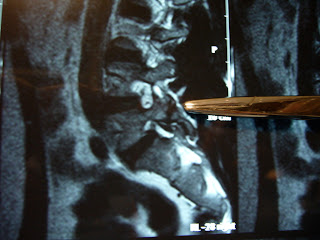
The MRI sagital reconstruction shows the small crack in the posterior elements, pointed out with the probe in the picture. Often these cracks are very hard, if not impossible to see on MRI, but might be picked up better on CT scan. “SPECT bone scans”, not just “whole body” bone scans are very sensitive for picking up even non-displaced or unilateral (one-sided) fractures.
In surgery today, it was amazing to see how loose the posterior L5 elements were. I was able to take out the entire posterior element structure, including the pars fracture, with only 2 bony pieces.
I spent some additional time clearing out the L5 neural foramen bilaterally, which is often “clogged” with reactive bone, ligament and disc, causing leg symptoms.
I also inserted a TLIF interbody cage in between the L5 and S1 vertebral bodies with local bone graft to provide better stabilization across the level we hoped would fuse.
The TLIF also helps to “jack open” the neural foramen.
The surgery went well, taking approximately 2 hours and 30 minutes, with subcuticular closure with Dermabond.
Estimated blood loss was less than 600 cc, and some blood was recycled using Cell Saver. No banked blood was used.
Postoperatively, he is recovering well up on the Duke Raleigh Hospital Orthopaedic Unit, and will get up and around tomorrow.
He is quitting smoking as of today with the help of Chantix and Nicotine patch, so his fusion will heal.
Spondyloloysis is on the differential diagnosis for back pain in kids and teenagers, and can sometimes be treated effectively in a Boston Brace if caught early.
Lloyd A. Hey, MD MS
Hey Clinic for Scoliosis and Spine Surgery
http://www.HeyClinic.com
Sunday, September 16, 2007
9 yo boy w/ severe spastic quadriplegia sp "shaken baby syndrome" and history thoracic fractures now with severe kyphosis and trouble sitting
He has gradually fallen into increasing severe kyphosis, with increasing difficulty sitting in wheelchair or any chair, and has obvious discomfort now sitting even less than an hour.
He has been braced, but it has become increasingly uncomfortable.
His sitting X-Rays from last year show 90 degree kyphosis which improves to 70 degree lying down.
New Xrays are pending.
Given his progressive symptoms and increasing trouble with sitting, I am considering trying to help this boy with a posterior instrumentation and fusion, possibly a Luque box, but he is obviously a high risk surgical candidate with his severe CP.
He is being cared for in a State nursing facility, with staff that all feel that he really needs to get some help, since it is affecting his daily life including feeding, etc.
I have sent his pictures to some of my friends in the Scoliosis Research Society (SRS) to get their input in this difficult case to help come up with the best solution for this boy.
Lloyd A. Hey, MD MS
Hey Clinic for Scoliosis and Spine Surgery
http://www.HeyClinic.com
Saturday, September 15, 2007
Poem from Postop Spondylolisthesis Patient to Dr. Hey: "It's great to be alive!"
I think this is only the second poem I have received in 12 years of practice, and this one is definitely a keeper.
I have, however, received at least a dozen excellent paintings and drawings and metal sculpture, along with countless small but special gifts that we have all over the office, except for a little Hawaiian Angel who sits over my desk at home, from my scoliosis patient from Hawaii.
Thanks so much, Irene, for your wonderful and heart-felt poem. You helped re-energize a tired surgeon at the end of a long week!
Dr. Hey
Hey Clinic for Scoliosis and Spine Surgery
http://www.heyclinic.com
______________________________
Irene’s Poem:
Here is Irene’s Introduction and Poem:
I told you yesterday that I was composing a poem for you and here goes. I will probably revise it a dozen times, but that’s neither here nor there….so far, this is it. Irene _______
Ode to Dr. Hey
Before the surgery on my back
The ability to walk I did lack.
The pain was bad in my ham strings
And my legs went numb among other things.
I had to sit in the nearest chair
And I said to myself, “This isn’t fair!”
So my hometown doc sent me for an MRI
And said surgery was want I should try.
And that’s when I met Dr. Hey
A spinal surgeon who knew the way
To get me back on the walking track
And did the surgery on my back.
I once called him a brag-a-dossious
That’s when my back felt so atrocious
But you’ve done your job once again
I’m walking now quite free of pain.
I thank the Lord for all your talents
The way you work and stay in balance
You talk of degrees and of surgery time
And of all the patients now that are doing fine
And that’s OK now since I have been there
It’s not just bragging, for I know you care.
And I sing the praises of your PA’s
I’ve called Jaclyn on many days
She assured me that things were going great
And each time I called I got her, no wait
So I thank you, Dr. Hey, with all my heart
You knew what to do right from the start…
So now at the age of seventy-five
I can say, “It’s great just to be alive!
Irene _______
Friday, September 14, 2007
Anterior/Posterior L5S1 Reconstruction for L5S1 Discitis likely secondary to Dental Infection. Sep 13 2007 Hey Clinic Surgery
My Hey Clinic and hospital staff rearranged my whole schedule for Thursday and Friday to help make room for this woman who was really suffering.
Yesterday, with the help of Dr. Chris Watters who performed the anterior approach, we removed the infected disc anteriorly, washed it out and packed it with bone graft.
I then turned her over and extended her fusion down to the iliac wings bilaterally.
Multiple cultures were sent off.
What can we learn:
Infections from one part of the body can spread through the body to other parts of the body, including the spine and discs.
Preventing infections from getting out of control is key.
Making sure you tell your doctor of all infections you have is very helpful when trying to determine cause of pain, and/or infection elsewhere.
Nell did great with her surgery yesterday. Her surgery was 5 hours, and she was resting comfortably in ICU last evening.
Notice on the X-Ray how I have two transverse cross-connectors, and then a third one parallel to the other rods. This helps prevent rod breakage. I also used the new stronger “Blue Rods” from Synthes, which are the latest in titanium alloy.
Many thanks to Sandra and Lawrence, who did wonderful job as scrub techs, and both stayed late.
Many thanks also to Jaclyn, my PA, who stayed late as well to help, and to Brittany who helped to get Nell admitted
Many thanks to Hey Clinic Team who made a next day front/back surgery happen including rearranging many patients.
Many thanks to the patients and their families who were willing to move their appointment so that Nell could get out of agony.
Lloyd A. Hey, MD MS
Hey Clinic for Scoliosis and Spine Surgery
Raleigh, NC USA
http://www.HeyClinic.com