This morning in surgery we helped a 39 yo gentleman with back and leg pain who had a chronic stress fracture, called a “spondylolysis” across his posterior elements known as the “pars”, of L5. He had failed conservative therapy, and his pain was greatly affecting his quality of life.
His X-Ray shows a slight lucency posteriorly at L5 where the stress crack is located, but it is hard to see.
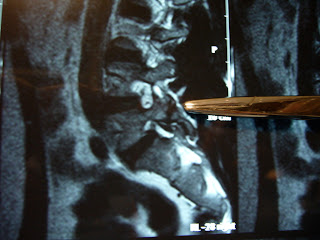
The MRI sagital reconstruction shows the small crack in the posterior elements, pointed out with the probe in the picture. Often these cracks are very hard, if not impossible to see on MRI, but might be picked up better on CT scan. “SPECT bone scans”, not just “whole body” bone scans are very sensitive for picking up even non-displaced or unilateral (one-sided) fractures.
In surgery today, it was amazing to see how loose the posterior L5 elements were. I was able to take out the entire posterior element structure, including the pars fracture, with only 2 bony pieces.
I spent some additional time clearing out the L5 neural foramen bilaterally, which is often “clogged” with reactive bone, ligament and disc, causing leg symptoms.
I also inserted a TLIF interbody cage in between the L5 and S1 vertebral bodies with local bone graft to provide better stabilization across the level we hoped would fuse.
The TLIF also helps to “jack open” the neural foramen.
The surgery went well, taking approximately 2 hours and 30 minutes, with subcuticular closure with Dermabond.
Estimated blood loss was less than 600 cc, and some blood was recycled using Cell Saver. No banked blood was used.
Postoperatively, he is recovering well up on the Duke Raleigh Hospital Orthopaedic Unit, and will get up and around tomorrow.
He is quitting smoking as of today with the help of Chantix and Nicotine patch, so his fusion will heal.
Spondyloloysis is on the differential diagnosis for back pain in kids and teenagers, and can sometimes be treated effectively in a Boston Brace if caught early.
Lloyd A. Hey, MD MS
Hey Clinic for Scoliosis and Spine Surgery
http://www.HeyClinic.com




No comments:
Post a Comment